|
In the first half of the previous century, tonsillectomy was the most frequently performed surgical procedure in America, and is still one of the most common today [1]. Yet surgical excision of the tonsils and/or adenoids is not as harmless or valid as commonly thought, and in this short article we’ll examine why.
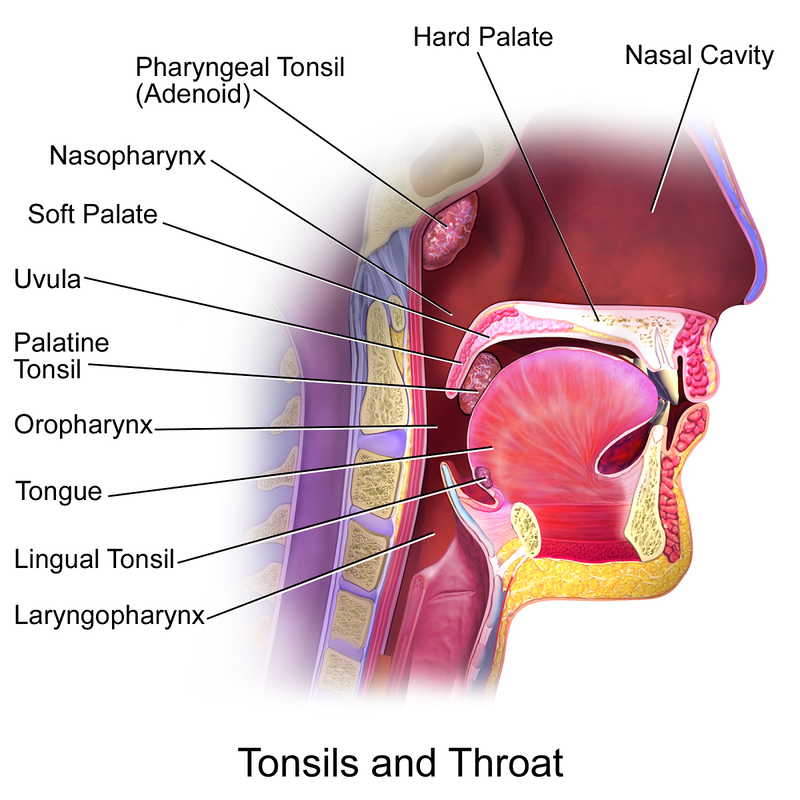
The palatine tonsils are the soft masses of lymphoid tissue located at the back of the throat that participate in both mucosal and systemic immunity [2]. The pharyngeal tonsils or adenoids are similar structures that can be found behind the nasal cavity. The adenoids and tonsils function as front line defenders against inhaled and ingested pathogens and the initial location for the generation of antigen-specific memory [3] [4]. Much like the appendix serves as a sentry for the colon, the tonsils serve as a sentry for the stomach, and with the appendix and tonsils both being components of the MALT (mucosa-associated lymphoid tissue), they are designed to work together [5] [6]. And tonsillar epithelial cells manufacture antimicrobial peptides termed defensins which play an important role in innate immune responses and help to shape the microbiota of the mouth [7]. Accordingly, drops in immunoglobulin levels after tonsillectomy may make vulnerable or predispose children to infectious diseases or allergic disorders, especially given that secretory IgA can be markedly reduced for more than 20 years after the tonsils are removed [8] [9] [10] [11]. We know that the tonsils play a large part in establishing and maintaining tolerance to allergens, and that deficiencies in vitamin A, vitamin D, and vitamin E are associated with the development of allergic disorders [12] [13] [14]. Specifically, vitamin D can increase the intratonsillar expression of the anti-inflammatory cytokine interleukin-37 (which helps modulate regulatory T cells and tolerance) as well as boost the production of the antiviral, antibacterial, and antifungal peptide LL-37 (also made by the tonsils) [15] [16] [17]. And vitamin A raises the tonsils’ crafting of interferon gamma, an immunomodulatory cytokine heavily involved in protection against viruses, bacteria, and protozoa [18]. The tonsils see their greatest immunological activity between the ages of 3 and 10, but childhood tonsillectomy is not without long-term consequence, as many conventionally-trained physicians still believe [19] [20]. In offering substantial examples as to why, a massive cohort study of almost 1.2 million children (published last year in the journal JAMA Otolaryngology – Head & Neck Surgery) revealed that having a tonsillectomy or adenoidectomy performed significantly heightened one’s risk for a range of respiratory, allergic, and infectious diseases (including asthma, pneumonia, influenza, chronic obstructive pulmonary disease, eczema, and urticaria or hives) [21]. Having the tonsils removed has also been associated with an increased risk of breast cancer and lymphoma, premature acute myocardial infarction (heart attack), Crohn’s disease, and appendicitis [22] [23] [24] [25] [26]. Rare complications of the tonsillectomy procedure itself include mediastinitis (inflammation of the mediastinum region between the lungs), Eagle syndrome (recurrent pain in the head and neck), atlantoaxial subluxation (partial dislocation among the first and second cervical vertebrae), and cervical osteomyelitis (infection of bone tissue in the cervical spine) [27]. Note that recurrent tonsillitis can be driven by upper cervical misalignment, so if this issue is present obviously it should be corrected before the tonsils are removed simply out of the diagnosis of recurrent tonsillitis [28]. Furthermore, let’s think for a minute – if the tonsils are repeatedly becoming inflamed, is it because they are dysfunctional, or is it because they are overwhelmed? If the tonsils are overwhelmed, will excising them eradicate the global burden on the immune system which overwhelmed them? Lastly, it is well known that between 1955 and 1963 both the oral and inactivated poliovirus vaccines were contaminated with simian virus 40 (SV40), a highly oncogenic DNA virus naturally hosted by rhesus monkeys that can induce the formation of tumors in brain, bone, lymph, and mesothelial tissue in humans [29] [30]. During the above time period, roughly 90% of children and 60% of adults in the United States were administered a poliovirus vaccine, and increased rates of multiple types of cancer have been found among those who were exposed to the contaminated vaccines [31] [32]. Most relevant to our interests is the fact that very clear evidence from research conducted decades ago (before the release of the Salk polio vaccine in 1955) demonstrated a significantly greater occurrence of bulbar poliomyelitis in those who had their tonsils removed versus those who had not [33] [34] [35]. In conclusion, I have not stated that the tonsils should never be removed. But the two main indications for tonsillectomy, recurrent throat infection and sleep-disordered breathing, are symptoms of deeper problems, and these deeper problems are not appropriately and completely remedied through focusing on the amelioration of enlarged tonsils. The tonsils and adenoids are laundering organs, so when morbid matter accumulates in the body, they can be called upon to assist in the elimination of refuse. Ergo, an overwhelming of the tonsils and adenoids will result in their congestion and inflammation. If congested and inflamed tonsils are extracted by an ENT, the body’s armament of laundering organs will be weakened, and remaining noxious material may find its way into the lungs or the gut. And this is why we find elevated incidences of respiratory and gastrointestinal ailments such as Crohn’s disease, appendicitis, asthma, pneumonia, and chronic obstructive pulmonary disease in those who have undergone a tonsillectomy. In vain does Nature protest against local symptomatic treatment, so please just be aware that a holistic and natural approach to improving the health of the body can prevent the need for a child’s tonsils to be taken out, despite the orthodoxy’s lack of understanding. References:
2 Comments
Denton
9/4/2020 20:53:45
Thank you!
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorDenton Coleman is an Exercise Physiologist and Medical Researcher. Archives
October 2023
Categories |

 RSS Feed
RSS Feed
